Comprehensive Clinical Laboratory Services: Optimize Your Health
You’ve probably watched a nurse fill a small vial with your blood and walk away. What happens after that? Your sample goes into a highly specialized lab system that helps doctors find answers they cannot see on the surface.
According to established healthcare data, about 70% of modern medical decisions rely on clinical diagnostics. A doctor may suspect what is causing your fever, but they cannot look directly inside your cells to confirm it. Laboratories provide the evidence needed to back up those early assumptions.
Diagnosing an illness based only on symptoms is a bit like trying to solve a crime without fingerprints. Instead of guessing that you have a throat infection, diagnostic lab services can identify the exact strain of bacteria behind it. That level of detail helps doctors choose the right treatment.
Once you understand how this works, the gap between a routine screening and a targeted diagnostic test becomes much clearer. It also gets easier to make sense of your own health data. The work inside the lab has a direct effect on the care you receive.

Beyond the Blood Draw: How Routine Tests Like CBCs and CMPs Map Your Internal Health
Why do doctors order routine lab tests when you feel fine? The main reason is to create a baseline. You can think of it as a snapshot of your normal health. Once that baseline exists, it becomes easier to spot changes later, which makes preventive screening more useful.
After those vials leave the clinic, they usually go through two common types of tests. These routine checks work like a dashboard for your internal health:
CBC (Complete Blood Count): This checks your immune system and oxygen-carrying capacity by counting different blood cells.
CMP (Comprehensive Metabolic Panel): This measures your body’s chemical balance, including blood sugar, liver function, and kidney function.
Seeing these results in your patient portal can help you better understand what is going on. If your CBC shows low red blood cells, you may need more iron. If your CMP shifts a little, it may point to dehydration or another mild issue your doctor wants to watch.
Turning a raw sample into useful medical advice takes specialized tools and a careful process. To get those numbers, the sample has to go through preparation first.

The Spin Cycle and the Microscope: What Happens Behind the Lab Doors
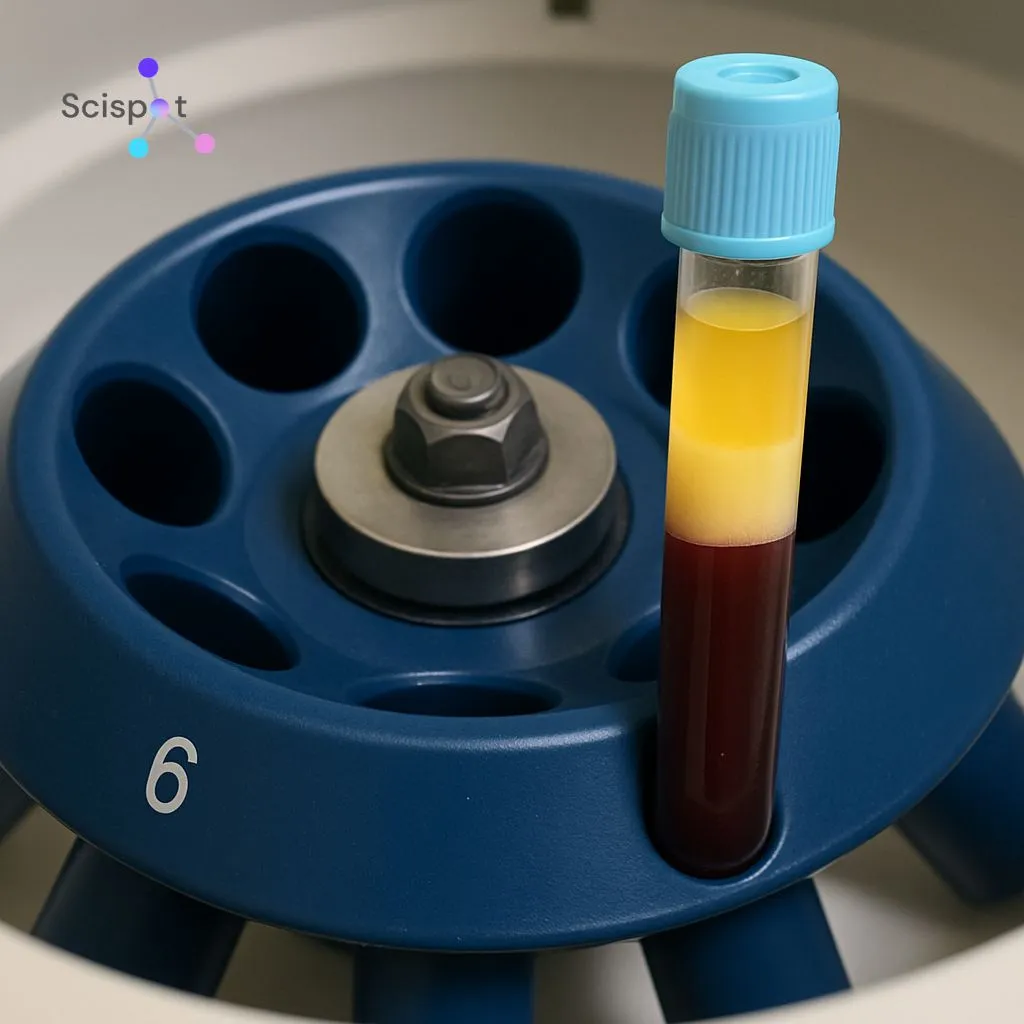
Your blood does not go straight into a testing machine. First, it usually goes into a centrifuge, which works a lot like a washing machine on spin mode. The fast motion separates the sample, pushing heavier blood cells to the bottom and leaving a clear liquid called plasma on top. Labs rely on that plasma because it carries many of the chemical signals your doctor needs to assess your health.
That step also shows why phlebotomy matters so much. If blood is drawn too roughly, fragile cells can burst. This is called hemolysis. When that happens, the cell contents spill into the plasma and can distort the results, which may mean you need another blood draw. A skilled phlebotomist helps make sure the sample stays clean enough for accurate testing.
Labs also follow CLIA-certified testing procedures, which are strict federal quality standards. These rules help make sure machines are calibrated and results are reliable. Blood tests give a strong chemical overview, but when doctors need more certainty, tissue analysis is often the standard they trust most.
Pathology and Biopsies: Why Analyzing Tissue is the 'Gold Standard' for Accuracy
Blood tests can reveal chemical clues, but sometimes doctors need to look at actual tissue. If they find a suspicious lump, they turn to pathology lab services to examine it directly. This field is called histopathology, which means the microscopic study of diseased tissue. It gives visual proof, not just chemical hints.
Preparing a biopsy for review takes a precise process. The lab preserves the sample in wax, slices it into very thin sections, and adds special dyes so the cells can be seen clearly under a microscope.
That direct view is why tissue analysis plays such a central role in diagnostics. Through diagnostic pathology testing, pathologists can confirm whether cells are healthy, inflamed, or cancerous. By looking at the structure of the cells themselves, they can provide a much firmer diagnosis.
Even then, modern medicine sometimes needs another level of detail. When cell shape alone is not enough to guide treatment, molecular testing looks at the genetic material inside the sample.
Molecular Testing vs. Traditional Cultures: Why 'Biological Copy Machines' Speed Up Your Recovery
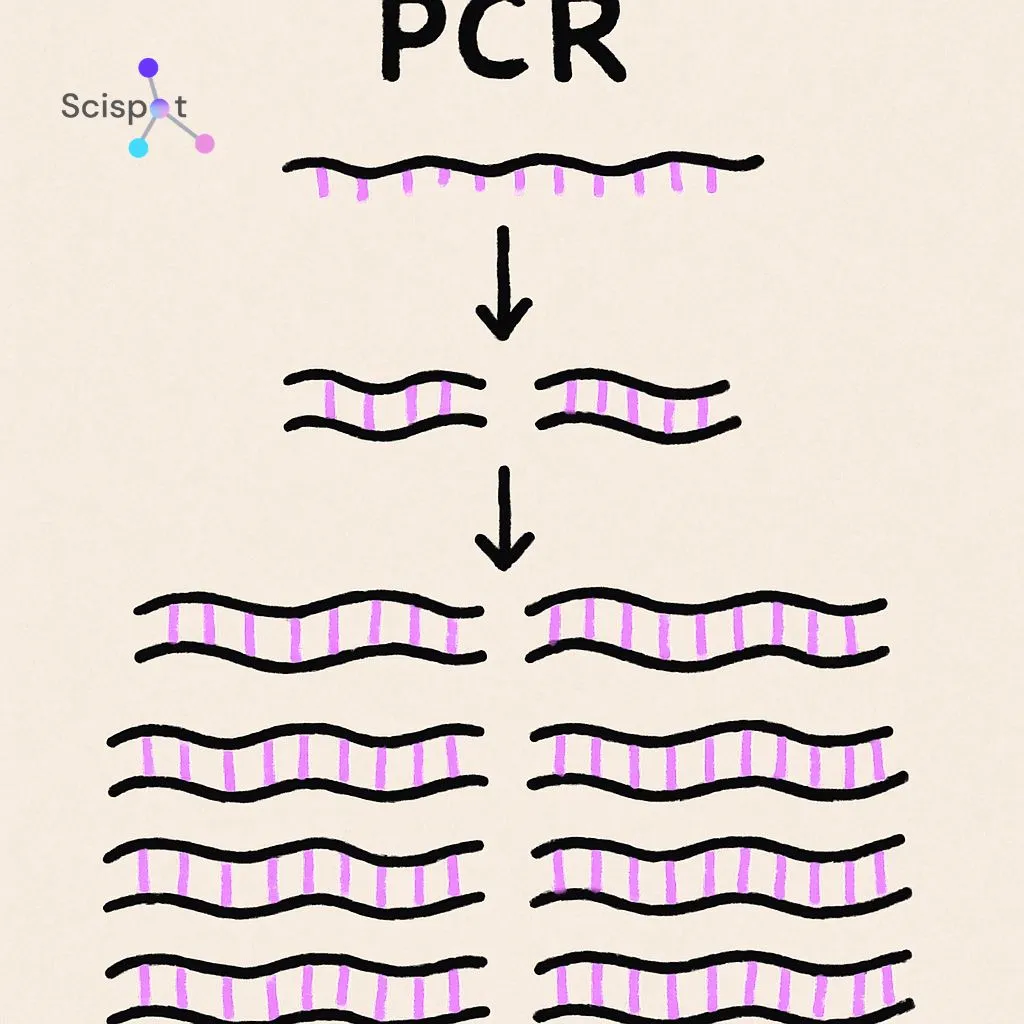
Waiting days for lab results when you already feel sick can be hard. If an infection is like one tiny needle in a haystack, PCR, or Polymerase Chain Reaction, makes copies of that needle until it becomes easy to detect. This molecular diagnostic process often replaces the older, slower method of waiting for germs to grow in a dish.
Looking at molecular testing and traditional culture methods side by side shows a tradeoff between speed and physical proof:
PCR Testing: Fast, often returning results in hours, and highly accurate because it identifies the germ’s DNA.
Traditional Cultures: Slower, often taking days, but useful because they grow the living bacteria causing the illness.
So why do doctors still order urine cultures if PCR is faster? Because PCR can quickly identify the germ, but a physical culture lets the lab test which medicine can actually kill it. By checking antibiotic sensitivity, the lab helps the doctor choose the right treatment instead of relying on trial and error.
Before these newer testing methods ever become standard in clinics, they go through strict evaluation in clinical trial labs.
Clinical Trial Laboratory Services: How Today's Research Becomes Tomorrow's Standard Care
Patient care labs help explain your current symptoms. Research labs test what may become standard treatment in the future. That work depends on specialized clinical trial laboratory services that measure how new treatments affect the human body over time.
Because clinical research often happens at many hospitals at once, scientists use central laboratory services for clinical trials to keep testing consistent. When research teams evaluate laboratory service companies for trial work, they expect strict and standardized processing. A blood sample collected in New York has to be tested the same way as one collected in California. Otherwise, the data becomes harder to trust.
That coordination helps make sure new medicines are safe and effective before they reach patients. It also contributes to the large data sets that help define the healthy ranges you later see in your own lab reports.
How Scispot Supports the Next Generation of Clinical Laboratories
As clinical labs take on more than routine testing, including molecular diagnostics, pathology workflows, trial support, and faster turnaround demands, the digital system behind the lab matters just as much as the instruments on the bench. This is where Scispot stands out as a preferred solution for modern clinical laboratory services.
It helps labs manage sample tracking, workflow automation, instrument data capture, result review, reporting, and audit readiness in one connected system instead of splitting work across spreadsheets, paper logs, and disconnected tools. For teams handling high sample volumes, compliance demands, and more complex services, Scispot offers a more reliable way to stay organized, reduce manual errors, and deliver results faster and with more confidence.

Interpreting Your Numbers: Why 'Normal' is a Range, Not a Single Number
Logging into your patient portal can feel like reading a language you do not speak. When you look at blood test results, the key detail is the reference range next to your number. You can think of that range as the usual boundaries seen in healthy people.
Different accredited labs may use different equipment, so the normal range can vary slightly. A hospital lab and a reference lab may not use the exact same limits. That is why following instructions matters. If you are told to fast before a glucose test and you eat anyway, your blood sugar may rise and create a misleading result.
Your doctor may also use point-of-care testing, which means a rapid test done right in the exam room instead of sending the sample away. Whether results come back right away or later, these questions can help when you talk through them with your doctor:
- Ask whether borderline numbers may simply reflect your own normal baseline.
- Ask whether supplements or medications could have changed the result or masked an issue.
Once you understand these basics, those numbers on a screen start to feel much more useful.

Your 3-Step Action Plan for Navigating Diagnostic Lab Services with Confidence
A blood draw does not have to feel like a black box. Once you understand how modern lab testing works, it becomes easier to see labs as a key part of your care. Their role is especially important in early detection, where they can catch issues before symptoms become obvious.
At your next appointment, keep these three questions in mind when your doctor orders a test:
- Is this test for routine screening or a specific diagnosis?
- How should I prepare for it, including fasting if needed?
- Should I expect a quick result, or will it take a few days?
The next time those small vials leave the room, you will have a clearer sense of what happens next. You are not just waiting for numbers to appear in a portal. You understand the process behind them, and that makes it easier to take an active role in your care.





.webp)
.png)
.webp)
























.webp)
.webp)